Total knee replacement is one of the most long-established and successful orthopaedic operations. More than 30,000 knee replacements are performed in the UK each year.
Total knee replacement is usually offered to patients with advanced arthritis, when symptoms can no longer be controlled with non-surgical alternatives. In these patients the surface cartilage in the knee has been worn away, often in more than part of the knee joint.
The goal of knee replacement is to provide a stable, pain-free joint.
Taken together, the surgeons at Castleview Clinic have performed several thousand total knee replacements. Each knee replacement is usually performed by a single surgeon, but at Castleview Clinic many are discussed between consultants before surgery to ensure the best outcome for each patient. Two consultants will often operate together in challenging cases, or when performing knee replacement on both knees simultaneously. All three surgeons can offer robotic-assisted total knee replacement to insured and self-pay patients.
Total knee replacement is one of the most long-established and successful orthopaedic operations. More than 30,000 knee replacements are performed in the UK each year.
Total knee replacement is usually offered to patients with advanced arthritis, when symptoms can no longer be controlled with non-surgical alternatives. In these patients the surface cartilage in the knee has been worn away, often in more than part of the knee joint.
The goal of knee replacement is to provide a stable, pain-free joint.
Taken together, the surgeons at Castleview Clinic have performed several thousand total knee replacements. Each knee replacement is usually performed by a single surgeon, but at Castleview Clinic many are discussed between consultants before surgery to ensure the best outcome for each patient. Two consultants will often operate together in challenging cases, or when performing knee replacement on both knees simultaneously. All three surgeons can offer robotic-assisted total knee replacement to insured and self-pay patients.
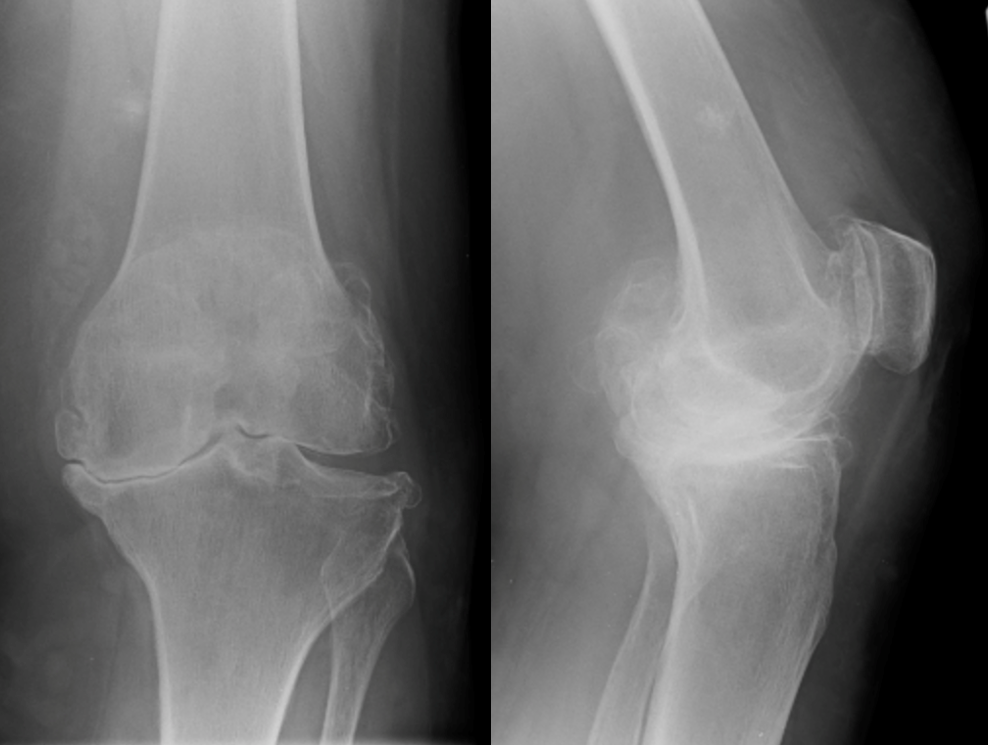
Advanced Osteoarthritis of the Knee
Symptoms and signs of advanced knee arthritis
Patients with advanced arthritis usually have significant pain, which is often worse when walking or at the end of the day. The worn, uneven joint surface may result in catching or locking, and the knee is often swollen.
These symptoms often wax and wane, but flare-ups may be felt more frequently as the cartilage wear progresses. Over time, the patient may notice that the knee becomes bowed or knock-kneed, and that the knee is stiff with difficulty fully straightening or bending.
Diagnostic Imaging
The worn cartilage in arthritis can usually be assessed with an x-ray. Although the cartilage is not visible, if the x-ray is performed with the patient standing, the bones will appear to touch in areas where the cartilage is very worn because there is no longer any cartilage separating them.
In a small number of cases an MRI scan is needed to fully evaluate the arthritis.
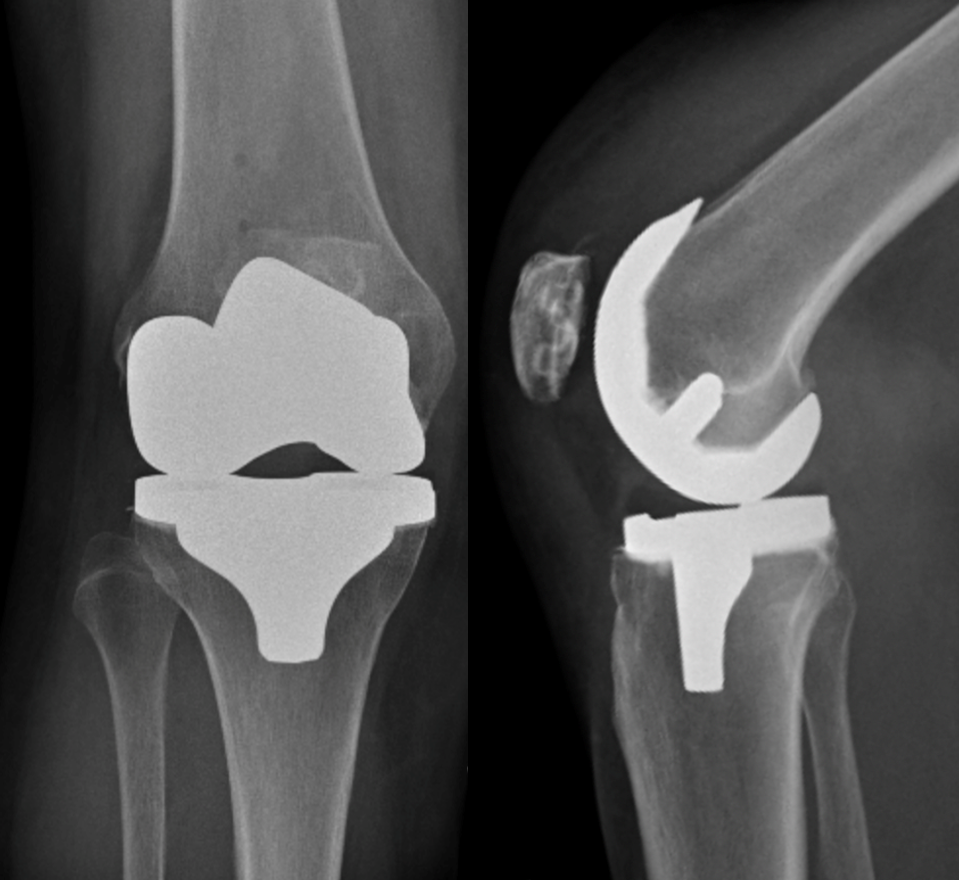
Total Knee Replacement
Diagnostic Imaging
The worn cartilage in arthritis can usually be assessed with an x-ray. Although the cartilage is not visible, if the x-ray is performed with the patient standing, the bones will appear to touch in areas where the cartilage is very worn because there is no longer any cartilage separating them.
In a small number of cases an MRI scan is needed to fully evaluate the arthritis.

Total Knee Replacement
Pre-Assessment
If total knee replacement is agreed upon, the next step will be attendance at a pre-assessment clinic. The pre-assessment is important to ensure any pre-existing medical conditions are identified or optimized to make the surgery and recovery as smooth as possible.
Hospital Stay
The patient is most often admitted on the day of surgery and most patients stay in hospital for one or two nights.
Anaesthesia
Knee replacement is most often performed using a combination of spinal anaesthesia, targeted nerve blocks and sedation. The spinal anaesthesia is similar to an epidural, and ensures the patient has no feeling below the waist for the duration of the operation.
High volume of local anesthetic is also injected all around the knee and lasts for several hours. In many cases the spinal anesthesia can be designed to wear-off quickly after the surgery to allow the patient to take their first steps on their new knee a few hours after the surgery. These options can be discussed with your consultant anaesthetist prior to surgery.
Surgical Technique
The surgery usually takes 60-90 minutes, but patients are normally away from the ward for two or 2 ½ hours to allow for anaesthesia and recovery.
The surgery is performed through a vertical incision at the front of the knee and the patella (knee-cap) moved to the side. Approximately 9mm of bone at the end of the femur (thigh bone), and 9mm at the top of the tibia (shin bone) are removed using precise instruments.
This bone is replaced with a metal cap on the end of the femur, and a metal tray on the top of the tibia. The metal components are held securely in place with bone cement. Two or three of the main ligaments around the knee are preserved.
A plastic liner is inserted between the components to allow the bones to move smoothly on each other. The undersurface of the patella (knee-cap) is usually replaced with a plastic button. The wound is closed with absorbable sutures below the skin.
The components are inserted to optimize alignment, fit, and the stability and balance of the patient’s own ligaments and soft-tissue around the knee. Robotic-assisted knee replacement allows for very accurate planning and execution of excellent alignment, fit and tissue balance.
Tourniquet
Knee replacement was traditionally performed with a tourniquet (blood pressure cuff) around the upper thigh. However, the surgeons at Castleview Clinic increasingly find that it can be done without tourniquet. This can significantly reduce early post-operative pain and means patients can walk on their new knee sooner.
Components
The surgeons at Castleview Clinic will select a highly-rated total knee replacement manufactured by Stryker, DePuy Synthes, Biomet or Implantcast. The UK National Joint Registry (https://www.njrcentre.org.uk/about-us/), and Orthopaedic Data Evaluation Panel (https://www.odep.org.uk/) monitor and benchmark the performance of all types of knee replacement in the UK. Please feel free to ask your surgeon at Castleview Clinic about the evidence that supports the implant chosen for your knee.
The components in all these brands are made from a metal alloy containing cobalt, chromium and very small amount (0.5%) of nickel. This alloy has been studied extensively over many decades and found to be an excellent choice for joint replacement because it is so inert and hard-wearing. The inclusion of nickel may concern a small number of patients who have previously had a skin reaction to nickel – please discuss this with your surgeon at your clinic appointment if you think it may affect you.
Post-operative recovery
Techniques for post-operative pain control have seen some of the most rapid advances in total knee replacement in recent years. Most patients can expect to be standing or walking on their new knee on the day of surgery under supervision of a physiotherapist. Most patients are ready to go home on the first or second day following surgery. Your anesthetist will discuss the right combination of pain relief for you to take in hospital and at home after surgery. One of the most significant recent advances is the use of “cryotherapy” – a cold sleeve wrapped around the knee to reduce pain, swelling and inflammation. This can be taken home after surgery and is strongly recommended.
When you go first go home, you will need to have made plans for someone to help you with daily activities like cooking, cleaning and washing. Your recovery will also be easier if you plan some adjustments to you home ahead of surgery. These might include a bench or chair in the shower, and a stable chair with a back, two arms and a firm seat cushion, along with a footstool to elevate your leg.
You will attend a nurse-led clinic two weeks following the surgery to review your wound. Outpatient physiotherapy begins within the first week after surgery. Please let your surgeon know where you will be attending physiotherapy after surgery to allow close communication with your physiotherapist. Your surgeon will usually see you at six weeks following the surgery.
Recovery following total knee replacement depends on a wide range of factors. As a general rule, we find that most patients use two crutches for up to two weeks, and use one crutch for up to six weeks. By six-week review almost all patients are walking without crutches. Most patients return to driving by 6-8 weeks after surgery.
Post-operative recovery
Techniques for post-operative pain control have seen some of the most rapid advances in total knee replacement in recent years. Most patients can expect to be standing or walking on their new knee on the day of surgery under supervision of a physiotherapist. Most patients are ready to go home on the first or second day following surgery. Your anesthetist will discuss the right combination of pain relief for you to take in hospital and at home after surgery. One of the most significant recent advances is the use of “cryotherapy” – a cold sleeve wrapped around the knee to reduce pain, swelling and inflammation. This can be taken home after surgery and is strongly recommended.
When you go first go home, you will need to have made plans for someone to help you with daily activities like cooking, cleaning and washing. Your recovery will also be easier if you plan some adjustments to you home ahead of surgery. These might include a bench or chair in the shower, and a stable chair with a back, two arms and a firm seat cushion, along with a footstool to elevate your leg.
You will attend a nurse-led clinic two weeks following the surgery to review your wound. Outpatient physiotherapy begins within the first week after surgery. Please let your surgeon know where you will be attending physiotherapy after surgery to allow close communication with your physiotherapist. Your surgeon will usually see you at six weeks following the surgery.
Recovery following total knee replacement depends on a wide range of factors. As a general rule, we find that most patients use two crutches for up to two weeks, and use one crutch for up to six weeks. By six-week review almost all patients are walking without crutches. Most patients return to driving by 6-8 weeks after surgery.
Complications relating to total knee replacement
These will be discussed with you by your surgeon in clinic and again on the day of surgery. Before your surgery we strongly recommend you review the information available on total knee replacement at https://www.consentplus.com. Your surgeon will be happy to discuss any particular concerns, especially those which may be individual to your case.
Outcomes after surgery
The goal of total knee replacement is to provide a knee that is pain-free and stable during all regular daily activities. In addition, patients are able to return to golf, skiing, and non-impact gym training. Many patients continue to play tennis, but most find that doubles tennis is more comfortable. Running, and high-frequency, high impact exercise is not recommended as it may shorten the longevity of the implant.
Over several decades, around the world, more than 85% of patients are satisfied with the outcome of their knee replacement. Since 2003, the National Joint Registry has allowed us to monitor the performance of each knee replacement in the UK. Among the modern, highly-rated implants used by the surgeons at Castleview Clinic, fewer than 5% of total knee replacements have been revised (re-done) within 15 years.
